If you’ve ever taken an over-the-counter antihistamine and felt a little better—but not fully better—you’re not alone.
Many women with
Or, if you are like me and some of my clients, they really did not help at all.
That’s because antihistamines are designed to manage symptoms, not resolve the underlying cause.
Let’s walk through why that matters.
👉Learn more about histamine intolerance.
Histamine Isn’t Just One Thing: Understanding the 4 Receptors
Histamine works by binding to four different receptors in the body—H1, H2, H3, and H4—and each one triggers a very different response depending on where it’s located.
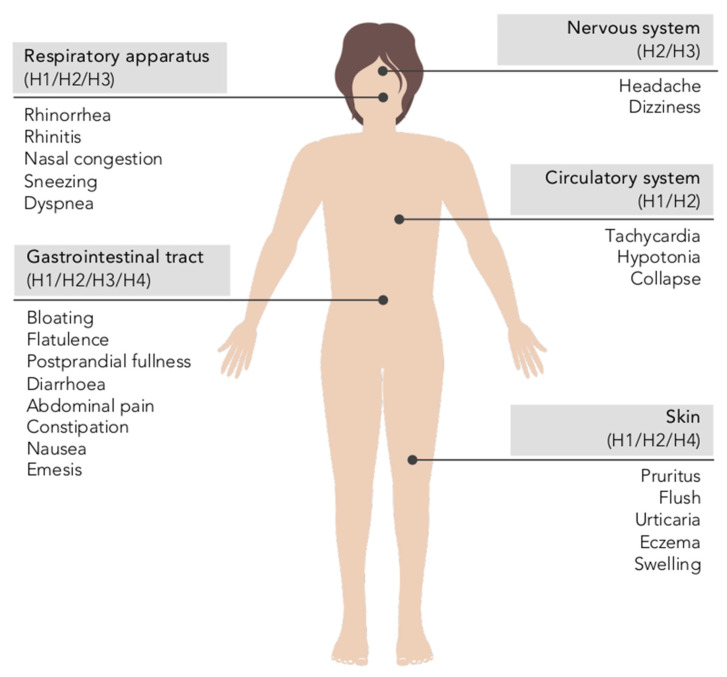
As shown in the Histamine Intolerance State of the Art graphic, these receptors are found throughout multiple organ systems, which helps explain why symptoms can feel so widespread and unpredictable.
H1 receptors: Linked to classic allergy-type symptoms like itching, hives, congestion, and inflammation
H2 receptors: Primarily found in the digestive system; stimulate stomach acid and may contribute to reflux or abdominal discomfort
H3 receptors: Located in the brain and nervous system; influence sleep, alertness, appetite, and headaches
H4 receptors: Involved in immune signaling and inflammation, especially in the skin and immune cells
Together, these receptors act like different “switches” for histamine throughout the body.
So, depending on which receptors are being activated—and where—you might experience skin reactions one day, digestive issues the next, or brain-related symptoms like anxiety or insomnia.
That’s why
Image courtesy Comas-Basté, O., Latorre-Moratalla, M. L., Bernacchia, R., et al. (2020). Histamine Intolerance: The Current State of the Art. Biomolecules, 10(8), 1181.
What Antihistamine Actually Do
OTC antihistamines, like loratadine or cetirizine, work by blocking histamine receptors—primarily the H1 receptor.
But when histamine levels rise too high, it can trigger symptoms like itching, headaches, congestion, flushing, and even anxiety or sleep disruption.
Antihistamines act by preventing histamine from binding to its receptor.
This can reduce symptoms fairly quickly, which is why they’re so commonly used for allergies. However, they don’t lower the amount of histamine in your body—they simply block its effects.
Think of it like putting a lid on a boiling pot. The steam may not escape as easily, but the heat underneath is still very much there.
Why They Help Some Women
For women whose symptoms are driven primarily by short-term histamine release—like seasonal allergies or environmental triggers—antihistamines can work quite well.
In these situations, histamine spikes temporarily, and blocking the receptor is often enough to provide relief.
If you have a tendency towards allergies, this can depend on your histamine genes and your gut health.
This is why you may notice improvement in symptoms like sneezing, itchy eyes, or hives when taking these medications. The issue is more about histamine signaling than histamine buildup.
Do OTC Antihistamines Work For Everyone?
Histamine intolerance is a different story.
Rather than a temporary spike,
For many women, this comes down to the enzyme diamine oxidase (DAO), which breaks down histamine in the gut.
When DAO activity is reduced—due to genetics, gut inflammation, medications, or nutrient deficiencies—histamine can accumulate and circulate throughout the body.
And this is where antihistamines fall short.
They don’t:
- Improve DAO activity
- Reduce histamine production in the gut
- Address imbalances in the microbiome
- Support detoxification pathways
- Correct underlying immune or inflammatory patterns
So while symptoms may feel slightly better, the root cause remains untouched.
This also explains why symptoms can feel unpredictable. Histamine affects multiple systems in the body, including digestion, the endocrine system, the immune system, and even the brain. That’s why one day it might be bloating and fatigue, and the next it might be headaches or early-morning insomnia.
To complicate matters, histamine-related conditions are influenced by a combination of genetic, environmental, and immune factors. These overlapping influences help explain why no single treatment works for everyone.
The Bigger Picture: It's Not Just Histamine
One of the biggest misconceptions about
In reality, it’s about how your body processes histamine.
Your gut plays a central role here. It’s not only where histamine from food is broken down, but also where certain bacteria can produce histamine. If the gut lining is compromised or the microbiome is imbalanced, histamine levels can rise even more.
Hormones also play a role. Many women notice their symptoms worsen at certain times in their cycle, particularly when estrogen is higher. This is because estrogen can influence histamine levels and the body’s response to it.
So when we zoom out,
A More Effective Approach
If antihistamines are the short-term fix, what does a long-term solution look like?
It starts with supporting your body’s natural ability to regulate histamine.
Natural antihistamines found in foods—like quercetin, sulforaphane, and vitamin C—work differently than medications. Instead of blocking receptors, they help stabilize immune cells and reduce histamine release.
At the same time, improving gut health is essential. This includes supporting the gut lining, encouraging a balanced microbiome, and ensuring your body has the nutrients it needs to produce enzymes like DAO.
A low-histamine diet is often used as a starting point, not as a permanent restriction, but as a way to reduce the overall load while the body heals.
One of the most powerful tools in this process is sulforaphane, a compound found in broccoli sprouts and other cruciferous vegetables.
Sulforaphane supports detoxification pathways, helps regulate inflammation, and promotes a healthier gut environment—all of which can improve how your body handles histamine over time.
👉Learn more about how sulforaphane can help you overcome allergies and more.

The Takeaway
OTC antihistamines can absolutely be helpful. They can provide relief during flare-ups and make symptoms more manageable in the moment.
But if you’re relying on them daily and still not feeling like yourself, that’s important information.
It suggests that your body may need more support—not just symptom control.
Histamine intolerance is complex, but it’s also highly responsive to the right approach.
When you focus on gut health, nutrient support, and targeted foods that work with your biology (not against it), you begin to shift from simply managing symptoms to actually improving your tolerance.
And that’s where things start to change in a meaningful, lasting way.
References
Comas-Basté, O., Latorre-Moratalla, M. L., Bernacchia, R., et al. (2020). Histamine Intolerance: The Current State of the Art. Biomolecules, 10(8), 1181.
Schnedl, W. J., & Enko, D. (2021). Histamine Intolerance Originates in the Gut. Nutrients, 13(4), 1262.
Yoshikawa, T., Nakamura, T., & Yanai, K. (2019). Histamine N-methyltransferase in the brain. International Journal of Molecular Sciences, 20(3), 737.
Maintz, L., & Novak, N. (2007). Histamine and
Schwelberger, H. G. (2010). Histamine intolerance: A metabolic disease? Inflammation Research, 59(Suppl 2), S219–S221.
Falcon, R. M. G., & Caoili, S. E. C. (2023). Immunologic, genetic, and ecological interplay of factors involved in allergic diseases. Frontiers in Allergy, 4, 1215616.