Are you struggling with chronic sinus issues, bloating, migraines, or insomnia, and wondering why nothing seems to help? You might be reacting not to a food allergy, but to a condition called histamine intolerance.
I know this firsthand. For years, one of my favorite indulgent meals was sausage pizza with a glass of red wine and dark chocolate for dessert. But without fail, I’d be wide awake that night with a pounding head and itchy skin. Eventually, I discovered the surprising culprit: histamine—a naturally occurring compound in many of our favorite foods.
In this blog, I’ll explain what
What is Histamine?
Histamine is a natural compound that plays essential roles in the body. It helps regulate digestion, works as a brain chemical (neurotransmitter), and is released by the immune system when you have an allergic reaction, infection, or injury.
You can think of histamine as a kind of “messenger molecule.” It tells your body when to make stomach acid, when to fight off an invader, and even helps regulate sleep and wakefulness. So, it’s essential—but too much of it can cause problems.
What is Histamine Intolerance?
Histamine intolerance (HIT) occurs when the body can’t efficiently break down histamine, whether from a diet high in histamine or from the histamine that our bodies produce.
This is unlike other food intolerances, like lactose intolerance, which is caused by a lack of the enzyme lactase and can easily be resolved by taking a digestive enzyme or consuming lactose-free dairy products.
Although the symptoms of
Typically, your body uses enzymes like DAO (diamine oxidase) and HNMT (histamine-N-methyltransferase) to break down histamine. DAO works mainly in your gut, breaking down histamine from food, while HNMT works inside your cells, managing histamine produced in the body.
But if either enzyme isn’t working well, histamine starts to build up, leading to a histamine flare, and symptoms like insomnia, headaches, or allergic-type reactions.
Symptoms: Why It's So Hard to Identify
One of the most frustrating parts of
Or, you could react with indigestion, especially heartburn and GERD. Even increased anxiety can be caused by high histamine levels.
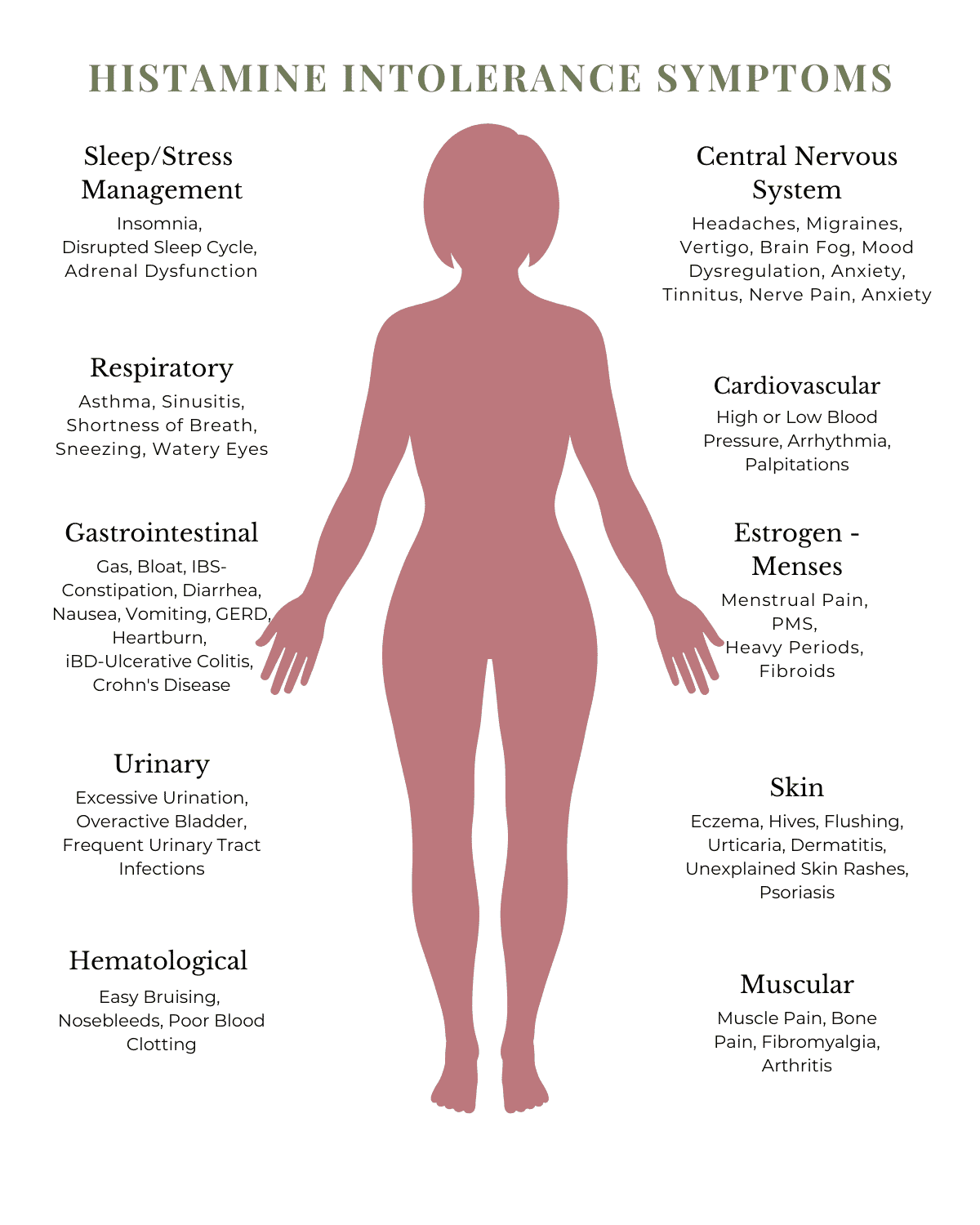
Common symptoms include:
- Bloating, gas, and diarrhea
- Indigestion, Heartburn, GERD
- Migraines and headaches
- Flushing, hives, or itchy skin
- Nasal congestion or sinus issues
- Insomnia, especially early morning insomnia
- Rapid heartbeat or low blood pressure
- Anxiety or irritability
This wide range of symptoms occurs because histamine acts on four different cell receptors (H1 through H4) found all over the body, from the brain to the gut to the skin.
For instance, the H2 receptors are found predominantly in the stomach and promote the production of stomach acid. This is why common antacids, like cetirizine, are referred to as H2 blockers.
What Causes Histamine Intolerance?
Because histamine plays so many different roles in our body, there are many causes of
For example, leaky gut or gut dysbiosis creates an immune response, increasing histamine and decreasing the production of the DAO enzyme. This is one reason that resolving
DAO Enzyme Deficiency
DAO is produced in the cells lining your small intestine; if your gut is inflamed or unhealthy, DAO levels drop. We also know that microbiome imbalances, including an overgrowth of histamine-producing bacteria, can reduce DAO enzyme.
You can also have a genetic variant in the DAO (AOC1), impacting your body’s ability to manage histamine levels.
Gut Microbiome Imbalance (Dysbiosis)
The gut microbiome plays a significant role. Certain gut bacteria can make histamine themselves, so an overgrowth of these bacteria or poor digestion overall can increase histamine levels.
In addition, gram-negative bacteria known as lipopolysaccharides (LPS) can increase inflammation and release of histamine.
Chronic Stress and Hormonal Imbalance
Stress hormones can trigger mast cells to release more histamine, especially during autoimmune flares or chronic anxiety.
Estrogen can also slow histamine breakdown, which may explain why many women experience symptoms around their cycle.
Consuming High-Histamine Foods
For decades, we’ve been eating high-histamine foods without even realizing it. Before refrigerators and freezers, people relied on methods like fermenting, smoking, and curing to keep food from spoiling, all of which increase histamine levels.
For example, dairy was often turned into yogurt through fermentation, and fish like salmon were smoked not just for taste, but to make it last longer. That’s why the highest histamine levels are usually found in aged, fermented, or preserved foods.
Examples include:
- Alcohol (especially wine and beer)
- Aged cheeses
- Fermented foods (like sauerkraut, kombucha, soy sauce, yogurt)
- Cured & preserved meats (like bacon, salami)
- Canned fish (like tuna or mackerel)
- Leftovers, especially meat leftovers (histamine increases as food sits)
Certain Medications
Some common medications block DAO activity, including certain antibiotics, antidepressants (like amitriptyline), and painkillers. While taking some of these medications on an occasional basis will unlikely cause
See my full list of medications that can impact histamine levels.
Intense or Prolonged Exercise
Exercise naturally triggers the release of histamine in your muscles, not because of an allergic reaction, but as a normal response to physical activity. Histamine plays a key role in regulating blood flow, inflammation, and recovery after exercise.
However, histamine can build up when you push your body too hard or don’t allow enough time to recover. This is especially true with weight-bearing or high-intensity workouts, which can lead to muscle damage and inflammation.
Over time, this may overwhelm your body’s ability to break down histamine properly, contributing to symptoms of
Genetics – Going Beyond DAO and HNMT Enzyme Genes
While you might have gene variants in the two main enzymes that break down histamine—DAO and HNMT—your body’s ability to handle inflammation and oxidative stress may have an even bigger impact on your
This is especially true if you’re dealing with an autoimmune condition like psoriasis or inflammatory bowel disease (IBD), including Crohn’s or ulcerative colitis.
For example, if your genes make it harder for your body to produce glutathione—a powerful antioxidant—it can reduce your ability to keep histamine levels in check. Learn more about histamine genes.
Histamine Intolerance Genomics Programs
Get down to the root cause of your histamine intolerance with genomic testing and evaluation. Programs include a comprehensive DNA Story consult more!
How Do You Know If You Have Histamine Intolerance?
Because the symptoms of
To complicate things, other food-related issues like lactose intolerance, glutamate sensitivity, sulfur intolerance, and even reactions to nightshade vegetables (due to solanine) can cause similar symptoms.
Food sensitivities—which are different from intolerances—can also show up in similar ways, including bloating, skin flare-ups, allergy-like reactions, and inflammation.
Right now, the most effective way to identify
While no lab test can confirm
How to Resolve Histamine Intolerance
Feeling overwhelmed by
With the right steps, you can reduce symptoms and even reintroduce favorite foods like yogurt or the occasional glass of wine.
But first, it’s important to know: there’s no such thing as a completely histamine-free diet. Nearly all foods contain some histamine or can trigger its release. The goal isn’t perfection—it’s learning what your body can handle and supporting it along the way.
Here’s how to get started:
✨ Follow a low-histamine diet for 30 days.
Use my Histamine Journal to track your food, symptoms, stress levels, and lifestyle habits, such as exercise and sleep.
🍽️ Need help in the kitchen?
Join my Cooking Low Histamine program to help you get started on a low-histamine diet and learn more on how you can resolve
💊 Support your body with DAO enzymes.
Try taking a DAO supplement like HistaHarmony before meals to help reduce symptoms while your body heals.
🧬 Look deeper with gut health testing.
My GI Spotlight Package includes gut microbiome and inflammation markers to uncover root causes like leaky gut—and create a personalized healing plan.
🧠 Ready to get personalized?
Sign up for one of my Histamine Gene programs to explore your genetic makeup and create a tailored plan to resolve
Final Thoughts
Histamine intolerance is real—and far more common than many people realize. If you’ve been dealing with confusing symptoms for years and haven’t found answers, histamine could be the missing link in your health journey.
Everything changed for me when I underwent genetic testing. That’s when I discovered why my body struggled to manage histamine levels. Yes, I had gene variants in both DAO and HNMT, but the real issue was deeper—my body’s reduced ability to manage inflammation and oxidative stress.
If this sounds familiar, you’re not alone. I’ve been there—and I’d love to help you get to the root cause and start feeling better. You can overcome
References
- Luttrell, M. J., & Halliwill, J. R. (2017). The intriguing role of histamine in exercise responses. Exercise and Sport Sciences Reviews, 45(1), 16–23. https://doi.org/10.1249/JES.0000000000000093:contentReference[oaicite:0]{index=0}
- Hrubisko, M., Danis, R., Huorka, M., & Wawruch, M. (2021). Histamine intolerance—The more we know the less we know: A review. Nutrients, 13(7), 2228. https://doi.org/10.3390/nu13072228:contentReference[oaicite:1]{index=1}
- Shulpekova, Y. O., Nechaev, V. M., Popova, I. R., Deeva, T. A., Kopylov, A. T., Malsagova, K. A., Kaysheva, A. L., & Ivashkin, V. T. (2021). Food intolerance: The role of histamine. Nutrients, 13(9), 3207. https://doi.org/10.3390/nu13093207:contentReference[oaicite:2]{index=2}
- Comas-Basté, O., Sánchez-Pérez, S., Veciana-Nogués, M. T., Latorre-Moratalla, M., & Vidal-Carou, M. C. (2020). Histamine intolerance: The current state of the art. Biomolecules, 10(8), 1181. https://doi.org/10.3390/biom10081181:contentReference[oaicite:3]{index=3}
- Schnedl, W. J., & Enko, D. (2021). Histamine intolerance originates in the gut. Nutrients, 13(4), 1262. https://doi.org/10.3390/nu13041262:contentReference[oaicite:4]{index=4}
- Jochum, C. (2024). Histamine intolerance: Symptoms, diagnosis, and beyond. Nutrients, 16(8), 1219. https://doi.org/10.3390/nu16081219:contentReference[oaicite:5]{index=5}







