What Your Dermatologist Is Not Telling You About Psoriasis
When it comes to psoriasis, the usual protocol is getting you started on a steroidal cream to calm down the inflammation allowing the skin to heal. Steroidal creams calm down the inflammation by suppressing your immune system.
Psoriasis is an autoimmune skin disorder where the immune system causes rapid skin cell growth. With healthy skin and normal skin cell growth, dead skin cells are sloughed off leaving, healthy new skin. However, with the rapid skin cell growth, the cells will begin to pile up, creating psoriasis plaques.
Steroid creams or immunosuppressant medications treat the symptoms and not the underlying cause of your psoriasis. One of the underlying causes of your flare or outbreaks can be your diet and nutrient deficiencies. Most dermatologists will not ask you about your diet and lifestyle habits. Except for limiting alcohol as this is a known trigger for psoriasis.
They also do not talk about food sensitivities and food intolerances. One food intolerance that has been shown to trigger or make psoriasis worse is
What are Some of the Most Common Triggers of Psoriasis?
Some of the most commonly known triggers of psoriasis are stress, alcohol, and certain medications. Injury to the skin as well as dry, cold weather can also trigger a flare or outbreak.
Ironically, both stress and alcohol can increase our levels of histamine. As a natural response, histamine is released when we under stress. Chronic stress will eventually lead to chronically high histamine levels.
Alcoholic beverages are high in histamine, as well as some of our favorite foods that go with alcohol like cheese, pizza, and preserved meats. There are many plant-based foods too that are high in histamine, including avocados, chocolate, and some nuts.
Is There a Difference Between a Food Intolerance and Food Sensitivity?
Food intolerances are usually due to a lack of enzymes that helps to breakdown and manage levels of certain compounds like lactose, histamine, and glutamate. Symptoms of food intolerances can vary greatly and usually involve headaches, allergic-type reactions, and digestive disorders.
On the other hand, food sensitivities are an immune reaction to certain sugars in foods. For instance, you may have developed a sensitivity to say soybeans, green peppers, or avocados. The most common symptoms of food sensitivities are digestive disturbances like IBS, heartburn, gas, and bloat.
The one food intolerance that can make psoriasis worse or increase flares is
What is Histamine Intolerance ?
Histamine intolerance is a food intolerance that is becoming increasingly more common. Like most food intolerances, it involves a lack of enzymes that help to breakdown compounds like lactose (milk sugar) and histamine from foods. With lactose intolerance, the symptoms usually involve digestive issues like diarrhea and gas. This is due to a lack of an enzyme called lactase.
Most food intolerances, once identified, can easily be managed by avoiding certain foods. Or, we can supplement with digestive enzymes like lactase. What makes
We become intolerant to histamine when we cannot correctly manage histamine levels resulting in a myriad of symptoms. As it is found in food and we produce it, it can be a challenge for some of us to keep histamine at manageable levels.
The cause of
Nutrigenomics or genetics also play a role, as there are gene variants in the production of enzymes that manage histamine levels.
This is why you will see symptoms like allergies and skin conditions run in families. See my Nutrigenomics Solutions for more information.
How Can Histamine Intolerance Make Your Psoriasis Worse?
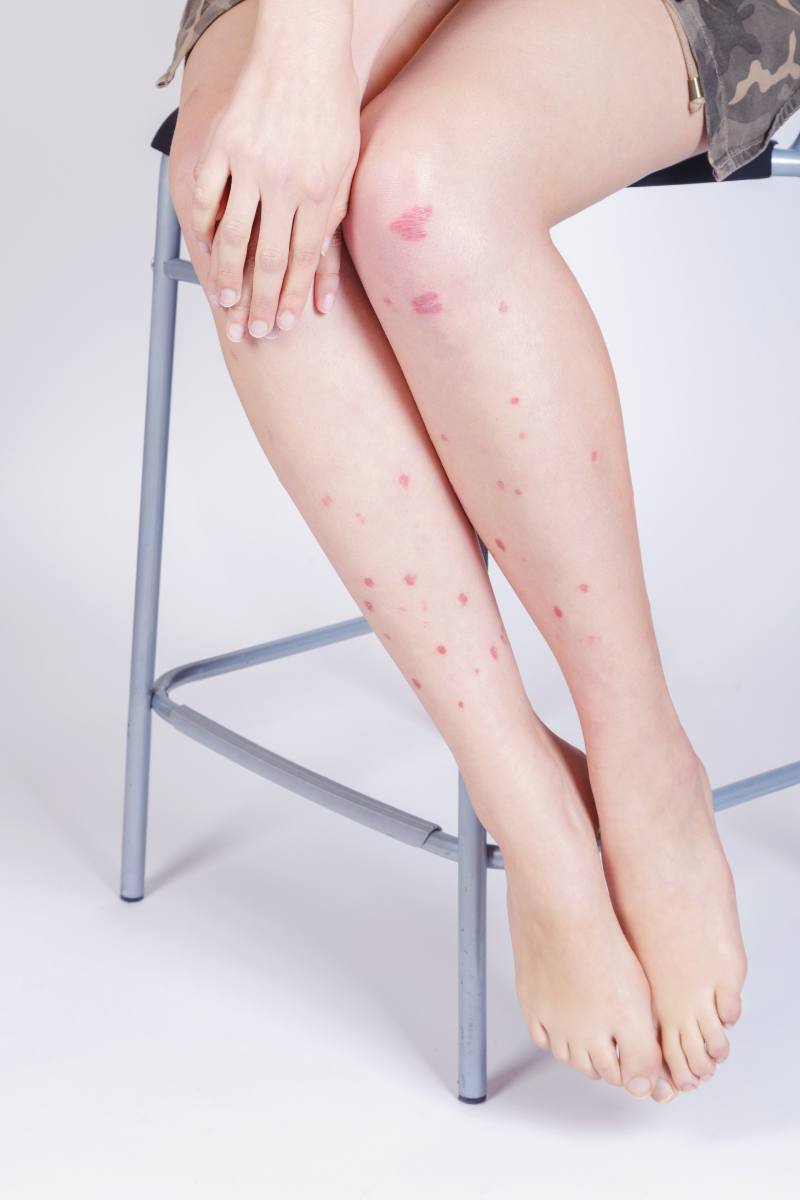
With a psoriasis outbreak or flare, your immune system will increase the production of histamine as a natural immune response. With the consumption of high histamine foods, your histamine bucket overflows, resulting in histamine intolerant symptoms like skin rashes, overreaction to bug bites, and other allergic-type reactions.
Studies have shown that take anti-histamine medication, like Benadryl, reduced psoriasis plaque as well as reduced the itchiness of psoriasis.
Anti-heartburn drugs like Tagamet have also been shown to reduce the severity of a psoriasis flare or outbreak. Tagamet is a H2 blocker that blocks the production of histamine, which plays a role in the production of stomach acid.
Another study found that the majority of patients with psoriasis were deficient in the enzyme known as DAO. This critical enzyme helps to block the absorption of histamine from food that we eat.
One of the major triggers of psoriasis outbreaks is excessive alcohol. Alcohol, as noted earlier, is high in histamine, especially beer. And, alcohol dramatically reduces the production of the critical enzyme, DAO. A double whammy!
Can You Test for Histamine Intolerance and Reduce Psoriasis Outbreaks?
One of the significant causes of
Currently, the best test for
The best way to determine if you are
Histamine intolerance can result in myriad symptoms and occur hours later after you consume high histamine foods. For me, my scalp psoriasis will get worse and itchier, after a high histamine meal, usually within 3-4 hours. Reminding me once to watch those histamine rich foods if I have a flare-up.
Can You Resolve Histamine Intolerance and Reduce Psoriasis Flares?
Unfortunately, you cannot treat food intolerances like
- Lack of enzymes – DAO, HMNT
- Nutrient Deficiencies (Folate, B12, Vitamin D, Vitamin B6, B2)
- Poor Gut Health or Leaky Gut
- Bacterial Imbalance or Dysbiosis
- Genetics
The first step, however, is to go on a low histamine diet. Remember, there is no such as a histamine free diet. See if this does help to reduce your flare or the frequency of your flares. If it does, then you need to get down to the underlying cause of why you are not correctly managing histamine levels.
As a functional medicine nutritionist, I use an integrative approach when reviewing lab work looking for nutrient deficiencies and imbalances. And, how we can finally resolve
References:
1. Efficacy of nutritional treatment in patients with psoriasis: A Case Report, Wong, et al August 30, 2014
2. Antihistamine in the treatment of pururitus in psoriasis, Domagata, et al, Advances in Dermatology and Allergogy 5, October, 2017
3. Psoriais and Diet, Part 1, Psoriasis Eczema Clinic, Australia Psoriasis Eczema Clinic, Accessed July, 2020
4. Histamine and